Normal xray of the hip xray4/20/2024  
In the absence of pathology, the two obturator foramen, ischial spines, greater and lesser trochanters and femoral heads should be symmetrical. Pelvis rotationĪn acceptable plain radiograph of the pelvis should be obtained with pelvis in a neutral position. In addition, the following factors should be considered. Images should allow for visualisation of the entire pelvis including the iliac crests, sacrum, sacroiliac joints, pubic and ischial rami, as well as the necks of the femora and the lesser and greater trochanters. When initially reviewing a plain radiograph of the pelvis, the radiograph should be assessed for adequacy. It can also be obtained in a weight-bearing manner, which may accentuate any arthritic changes, and give an indication of limb length discrepancy. The AP pelvis X-ray can be performed in a supine position, with efforts made to control the pelvic tilt and rotation, enabling similar radiographs to be obtained in every patient. Acetabular and femoral parameters that are assessed on plain radiographs are then described.Ī plain antero-posterior (AP) radiograph of the pelvis facilitates an assessment of each hip joint on an individual basis, as well as allowing for a comparison to be made to the contra-lateral hip joint. This article aims to summarise the most important aspects of the assessment of plain radiographs performed on the young adult hip joint. This paper begins by describing the parameters that potentially impact the quality of antero-posterior (AP) and lateral radiographs of the hip, and the variations in lateral radiographs that can be used. Radiographic examination remains the mainstay of the initial assessment however, common parameters are required to assist in the formation of accurate diagnoses and appropriate management plans including appropriate further imaging. doi:10.1148/rg.An enhanced awareness of the presence of structural disorders of the hip, such as developmental dysplasia of the hip and femoroacetabular impingement (FAI), has fuelled an evolution in the assessment of patients with hip pain and enhanced our ability to diagnose patients, even in cases where there are mild structural abnormalities. Imaging of the Pubic Symphysis: Anatomy and Pathologic Conditions. MRI Diagnosis of Subpubic Cartilaginous Cyst. Athletic Pubalgia and "Sports Hernia": Optimal MR Imaging Technique and Findings. Atlas of Normal Roentgen Variants That May Simulate Disease E-Book. The Adult Human Pubic Symphysis: A Systematic Review. Diseases of the Pubis and Pubic Symphysis: MR Imaging Appearances. Supplied by branches of the pudendal and/or genitofemoral and/or iliohypogastric/ ilioinguinal nerves 2Ĭongenital widening of the pubic symphysis (rare) 5ĭue to anteriorly-situated secondary ossification centers may appear "V-shaped" in adolescents on axial slices but will normally be parallel in adults 1 Mainly supplied by branches of obturator and inferior epigastric arteries 2 Normally very little movement: up to 2 mm shift and 1° rotation 2. Proximal ends of the penile/clitoral shaftsīladder (separated from the pubic symphysis by the retropubic fat pad) Remaining thigh adductor muscles (adductor magnus, pectineus, gracilis) 7 Remaining anterior abdominal wall muscles (internal oblique, transversus abdominis) 7 Other ligaments which attach to the pubic symphysis include:Īdductor longus, adductor brevis and rectus abdominis muscles attach to the anterior pubic ligament and interpubic disc 2Įxternal oblique aponeurosis also reinforces the pubic symphysis anteriorly 3 Posterior pubic ligament: blends with periosteum of both pubic bodies posteriorly 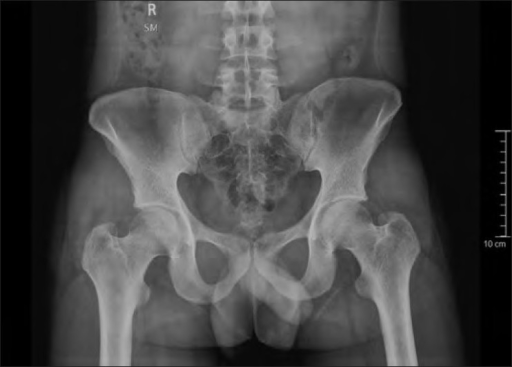
Inferior pubic (or subpubic or arcuate) ligament: runs from right to left inferior pubic ramusĪnterior pubic ligament: blends with periosteum laterally as well as the interpubic disc Superior pubic ligament: runs from pubic crest to pubic crest The pubic symphysis is reinforced by four strong ligaments 2,3: The width of the joint space differs at different ages:įor physiological reasons, women have a greater thickness of the fibrocartilaginous disc, allowing more mobility of the pelvic bones and thereby providing a larger pelvic diameter needed for childbirth. The pubic symphysis is a secondary cartilaginous joint, which means there is a wedge-shaped fibrocartilaginous interpubic disc situated between two layers of hyaline cartilage, which line the oval-shaped medial articular surfaces of the pubic bones 1,2. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
